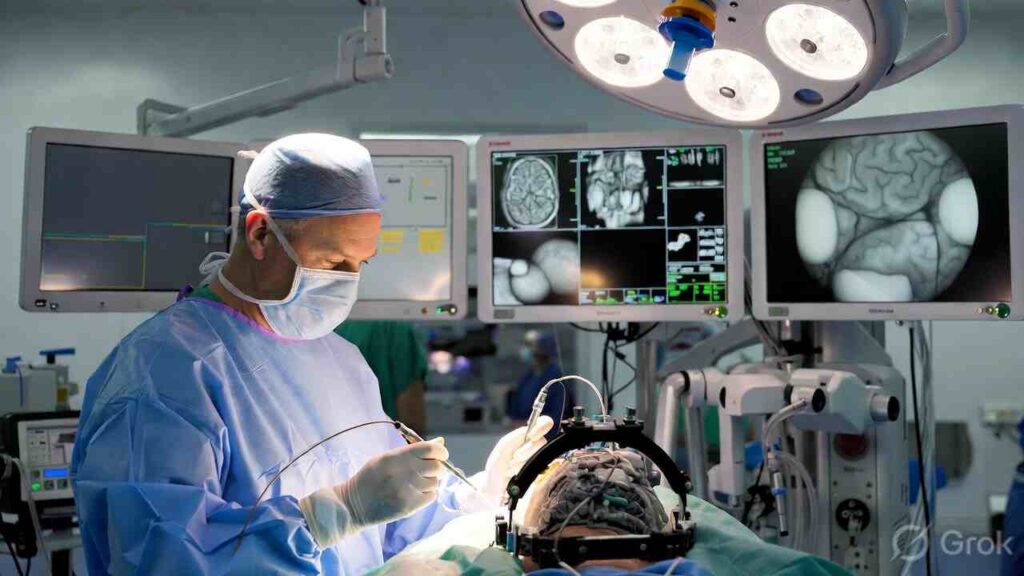
Advances in surgical technology have transformed the field of neurosurgery. Among the most significant advancements is minimally invasive brain surgery, a suite of procedures that reduce trauma to healthy tissue, shorten recovery times, and improve outcomes for many patients with neurological conditions. While traditional open craniotomy surgery remains essential in many cases, minimally invasive approaches are now indicated for tumors, hemorrhages, vascular abnormalities, epilepsy, and spinal conditions.
However, navigating the world of minimally invasive brain surgery can be overwhelming for patients and families. Decisions must be made about which surgeon to trust, the type of technology used, and — critically — the cost of care. This guide provides a thorough explanation of minimally invasive brain surgery, leading surgeons in the field, cost considerations in different regions, factors influencing pricing, success rates, risks, recovery expectations, and how to select the right clinic and surgeon for your situation.
1. What Is Minimally Invasive Brain Surgery?
Minimally invasive brain surgery refers to neurosurgical techniques that achieve therapeutic goals through smaller incisions, limited disruption of surrounding tissues, and less exposure of the brain compared to traditional open surgery. These methods use advanced imaging, small operative tools, and innovative approaches such as endoscopy, keyhole craniotomies, laser ablation, and navigation systems.
A. Key Principles
Minimally invasive techniques focus on:
- Reduced surgical trauma
- Smaller incisions
- Improved visualization using high‑definition cameras
- Precise, targeted intervention
- Faster recovery
- Lower complication rates
Instead of a large opening in the skull, surgeons can operate through tiny ports or natural pathways to remove tumors, relieve pressure, or repair vascular problems.
B. Common Indications for Minimally Invasive Brain Surgery
Minimally invasive brain surgery may be used for:
- Brain tumors (benign or malignant)
- Epidural or subdural hematomas
- Aneurysms and vascular malformations
- Hydrocephalus (fluid buildup)
- Epilepsy treatment
- Pituitary gland surgery
- Spinal cord compression or spinal tumors
Each condition requires specific approaches and technologies tailored to the individual’s anatomy and pathology.
2. Technology and Techniques in Minimally Invasive Brain Surgery
Modern neurosurgery depends on integrated technologies that enhance precision and safety.
A. Endoscopic Neurosurgery
Endoscopes are thin tubes with high‑resolution cameras that allow surgeons to see deep inside the brain through small openings.
- Transnasal endoscopy: Often used for pituitary tumors through the nasal passages, eliminating external incisions.
- Endoscopic third ventriculostomy: A minimally invasive procedure for treating hydrocephalus.
B. Keyhole Craniotomy
Rather than opening a large section of the skull, surgeons create a small “keyhole” opening — sometimes only a few centimeters in size — providing access to specific brain regions with minimal disruption.
C. Stereotactic Navigation
Advanced navigation systems use preoperative imaging to guide instruments precisely, similar to a GPS system for the brain.
D. Intraoperative Imaging
Intraoperative MRI or CT scans provide real‑time imaging during surgery, enabling adjustments for maximum accuracy.
E. Laser Interstitial Thermal Therapy (LITT)
This minimally invasive technique uses laser energy delivered through a small probe to destroy tumors or epileptic foci with minimal damage to surrounding tissue.
3. Minimally Invasive vs. Traditional Brain Surgery
| Feature | Traditional Open Surgery | Minimally Invasive |
|---|---|---|
| Incision size | Large | Small (keyhole or port) |
| Tissue disruption | Significant | Minimal |
| Visual guidance | Direct view | Endoscopic/Navigation systems |
| Recovery time | Longer | Shorter |
| Hospital stay | Extended | Often shorter |
| Scarring | More visible | Minimal |
| Complication risk | Higher | Lower (in many cases) |
While minimally invasive approaches are preferred where appropriate, not all conditions can be treated this way. Complex tumors encasing critical vessels or large hemorrhages often still require traditional surgery.
4. Leading Minimally Invasive Brain Surgeons
Choosing the right neurosurgeon is one of the most important decisions a patient will make. Below are highly respected surgeons and contributors in minimally invasive brain surgery — recognized for clinical excellence, research contributions, and leadership in the field.
A. Dr. Michael Lim
A pioneer in minimally invasive neurosurgery, particularly in endoscopic and keyhole techniques. Known for combining surgical skill with advanced technology to achieve precise tumor access through small openings.
B. Dr. Alfredo Quiñones‑Hinojosa
Renowned for his work with brain tumors and complex neurosurgical procedures. He has contributed to research and teaching on advanced surgical techniques, including minimally invasive approaches.
C. Dr. William Couldwell
A national leader in neurosurgical oncology and minimally invasive pituitary surgery. His expertise includes use of endoscopy and navigation systems to enhance precision.
D. Dr. Mitchel Berger
Known for complex brain tumor resections, including minimally invasive strategies when appropriate, and leadership in neurosurgical education.
E. International & Regional Experts
In addition to U.S.-based surgeons, many specialists worldwide — including those in Europe, Asia, and Australia — have distinguished reputations in minimally invasive neurosurgery, especially in endoscopic skull base surgery and laser therapies.
5. Cost of Minimally Invasive Brain Surgery
Costs vary significantly by region, hospital, surgeon experience, technology used, and complexity of the condition being treated. Below is a general breakdown of typical costs seen in 2026:
A. In the United States
Minimally invasive brain surgery in the U.S. is among the most expensive due to advanced technology, facility fees, physician expertise, and comprehensive care protocols.
| Cost Component | Typical Range |
|---|---|
| Pre‑operative evaluation & imaging | $1,500 – $4,500 |
| Surgeon fees | $10,000 – $25,000+ |
| Hospital charges (operating room + monitoring) | $30,000 – $60,000+ |
| Anesthesia fees | $2,000 – $6,000 |
| Navigation/Imaging systems | $5,000 – $15,000 |
| Post‑operative stay & rehabilitation | $10,000 – $30,000+ |
| Total Estimated Cost | $60,000 – $150,000+ |
B. In India
India offers world‑class neurosurgical care at a fraction of the cost compared to Western countries. Many patients from abroad choose India for both quality and affordability.
| Cost Component | Typical Range (INR) | Approx. USD |
|---|---|---|
| Pre‑operative evaluation | ₹30,000 – ₹75,000 | $350 – $900 |
| Surgeon fees | ₹1,00,000 – ₹4,00,000 | $1,200 – $4,800 |
| Hospital & OR charges | ₹3,00,000 – ₹10,00,000 | $3,500 – $12,000 |
| Anesthesia fees | ₹50,000 – ₹1,50,000 | $650 – $1,800 |
| Navigation/Imaging support | ₹50,000 – ₹2,00,000 | $650 – $2,400 |
| Post‑operative care & rehab | ₹1,00,000 – ₹5,00,000 | $1,200 – $6,000 |
| Total Estimated Cost | ₹6,00,000 – ₹20,00,000 | $7,000 – $24,000 |
C. Europe & Middle East
Costs in Europe and the Middle East generally fall between Indian and U.S. pricing, with many advanced centers offering minimally invasive surgery in high‑tech facilities.
| Region | Estimated Total Cost (USD) |
|---|---|
| Western Europe | $40,000 – $90,000 |
| Middle East | $30,000 – $80,000 |
| Eastern Europe | $25,000 – $60,000 |
Key Takeaway: India provides the most cost‑effective option without compromising on clinical expertise or outcomes, while the USA offers cutting‑edge technology at higher costs.
6. What Determines the Price?
A. Complexity of Condition
Simple procedures such as small superficial tumors or select endoscopic surgeries are less expensive than complex skull base tumors or vascular repairs.
B. Technology Used
Navigation systems, intraoperative imaging, and laser ablation add to expenses, but also improve precision and outcomes.
C. Hospital Level
Tertiary care hospitals with intensive monitoring units and multidisciplinary support charge more than smaller surgical centers.
D. Surgeon Reputation & Experience
Surgeons with national or international recognition may command higher fees due to expertise and proven outcomes.
E. Pre‑ and Post‑Operative Care
Comprehensive evaluations, rehabilitation, and long‑term follow‑up add to the total cost but enhance safety and recovery prospects.
7. Outcomes & Success Rates
Minimally invasive brain surgery has demonstrated improved outcomes in many scenarios:
- Reduced hospital stay: Many patients are discharged faster than with traditional open surgery.
- Lower complication rates: Smaller incisions and less tissue disruption correlate with fewer infections and reduced blood loss.
- Faster recovery: Patients often experience quicker return to daily activities.
- High precision: Navigation and visualization systems enhance accuracy in targeting pathology while preserving healthy tissue.
Success depends on individual diagnosis, age, overall health, and how early the condition is treated.
8. Risks and Complications
All surgery carries risk. Minimally invasive brain surgery reduces but does not eliminate them.
Common Risks
- Swelling or inflammation
- Headache
- Temporary neurological symptoms
- Infection
Serious but Rare Complications
- Bleeding in the brain
- Stroke
- Seizures
- Permanent neurological deficits
Risk Reduction Strategies
- Thorough pre‑operative evaluation
- Selection of specialized surgeons and high‑volume centers
- Advanced imaging before and during surgery
- Meticulous postoperative care
9. Recovery After Minimally Invasive Brain Surgery
Recovery varies with the procedure type, location of surgery, and individual patient factors.
Immediate Post‑Op Phase (Day 1–3)
- Pain management
- Rest and monitoring
- Early mobilization when appropriate
Early Recovery (Week 1–3)
- Restricted activities
- Follow‑up imaging
- Monitoring for signs of infection or complication
Mid‑Stage Recovery (1–3 Months)
- Gradual return to light work or daily activities
- Physical or occupational therapy if indicated
Long‑Term (3–12 Months)
- Full recovery in many cases
- Continued follow‑up for underlying conditions
Patients are advised to avoid heavy lifting, strenuous exercise, or contact sports until cleared by the surgeon.
10. How to Choose the Right Surgeon and Clinic
Patients should consider:
A. Surgeon Experience
Look for neurosurgeons with:
- Fellowship or specialized training in minimally invasive techniques
- High procedural volumes
- Documented outcomes
B. Technology Availability
Advanced imaging, navigation systems, and intraoperative tools enhance precision.
C. Multidisciplinary Support
Teams including neurologists, radiologists, anesthesiologists, and rehabilitation specialists improve holistic care.
D. Transparent Pricing
Understand exactly what is included — pre‑op tests, surgeon fees, OR charges, post‑op care, and rehabilitation.
E. Patient Testimonials & Reviews
Real patient perspectives help gauge satisfaction and outcomes.
11. Insurance and Financing Options
In the USA
- Most patients rely on insurance coverage for medical necessity — including tumor resection and vascular surgery.
- High deductibles and co‑pays may still apply.
- Hospitals may offer payment plans.
In India
- Limited insurance coverage for surgery; many patients pay out‑of‑pocket.
- Some hospitals offer EMI financing or cashless arrangements for international patients.
Medical Loans
- Many patients use specialized medical loans to finance complex procedures when immediate payment is difficult.
12. Patient Stories and Real‑World Perspectives
Real experiences help illustrate what patients can expect:
Case 1: Tumor Removal with Endoscopic Approach
A 42‑year‑old presented with headaches and vision changes. Minimally invasive endoscopic surgery successfully removed the lesion through a small nasal corridor. The patient was discharged within three days and returned to work within two weeks.
Case 2: Keyhole Resection for Localized Tumor
A 55‑year‑old with a benign brain tumor underwent keyhole craniotomy. Advanced navigation allowed precise resection; the patient experienced no major deficits and returned to normal activities within six weeks.
13. Future of Minimally Invasive Neurosurgery
The future holds promise:
- Robotic assistance
- AI‑enhanced imaging
- Improved laser and ablation systems
- Personalized surgical planning
These technologies will continue to increase precision and safety while reducing recovery time.
14. Conclusion
Minimally invasive brain surgery represents a major leap forward in neurosurgical care. The use of advanced imaging, endoscopic visualization, navigation systems, and precise tools allows surgeons to treat complex conditions while minimizing trauma to healthy tissue.
Choosing the right surgeon and clinic — based on expertise, outcomes, technology, and cost — is essential to achieving the best results. Although prices vary widely between countries and facilities, patients have options: high‑tech centers in the United States, cost‑effective world‑class care in countries like India, and competitive alternatives across Europe and the Middle East.
Patients and families should engage in open discussions with experienced neurosurgeons, understand the full scope of costs, and plan recovery and financing for the best possible outcome.
Your health, function, and quality of life depend not just on the surgical procedure — but on the experience, preparation, and care that surround it.